02
May
2024
How can we ensure that people for Microsclerotherapy are appropriately selected, consented and treated in a safe environment with oversight by a healthcare professional?
Competence is more important than qualifications
You might think that the question of who can inject leg spider veins is a battle between doctors, nurses and aesthetic practitioners.
Well it’s not and I am going to tell you why.
I am going to tell you who I think can inject leg spider veins and if you read to the end, I’ll tell you why I think the current system in the United Kingdom may change…soon...and for the better.
But before that, let me point you to the latest expert guidance on Microsclerotherapy. It was published at the end of 2023, so it’s really up to date.
I've read it carefully and I agree with following:
-1) “If C1 disease is not accompanied with symptoms consistent with venous disease, duplex ultrasound is not required and investigation of abnormal venous haemodynamics with duplex ultrasound should be reserved for symptomatic patients only.”
This means that if your patient only has spider veins, a duplex scan is not required. I agree and I cover this in detail in my course.
-2) “...it is advised that the minimum effective concentration and lowest volume of sclerosant is used at each injection site.”
Again, this is something I totally agree with.
-3) "The suggested concentrations of sclerosant are 0.25% polidocanol and 0.1% sodium tetradecyl sulfate for spider veins."
Again, I totally agree.
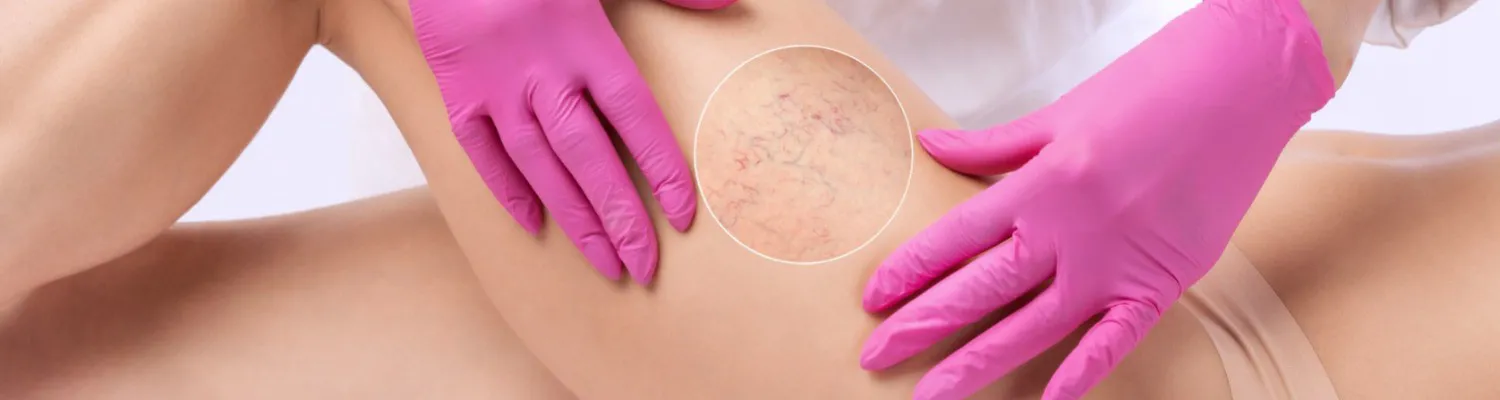
For those who are not familiar with Microsclerotherapy, let me bring you up to speed... it involves using a very fine needle (hence the micro-bit) and a prescription medicine called a sclerosant (hence the sclerotherapy -bit). The sclerosant is injected into the spider vein.
Successful injection is confirmed by the displacement of blood in the vein, resulting in a visual phenomenon called blanching.
Microsclerotherapy requires training, skill and practice, so if the injector is appropriately trained and is competent, it really doesn’t matter whether the injector is a doctor, nurse or non-medical practitioner.
In fact, my hands-on course accepts non-medical practitioners provided that the practitioner works under the supervision of a healthcare professional who prescribes the sclerosant after assessing the patient.
The important aspects of treating people with leg spider veins are as follows:
The patient is carefully assessed by history and examination
Account is taken of the indication and contra-indications
The patient is carefully consented
The practitioner is able to provide appropriate aftercare
The practitioner can manage anaphylaxis (a very rare complication of sclerotherapy)
The practitioner has access to advice and can refer for a second opinion
Regulation of Microsclerotherapy in the UK may be just around the corner….
Last year, the UK government held a consultation on the regulation of all cosmetic procedures. It has been proposed that Microsclerotherapy is an “Amber Procedure” with medium risk of complications. It also proposed in this consultation that for Microsclerotherapy,
"Aesthetic practitioners must have relevant oversight by a named regulated healthcare professional (who has gained an accredited qualification to prescribe, administer and supervise aesthetic procedures). "
In the UK, both licensed sclerosants are prescription only medicines which means only doctors and dentists can prescribe along with Nurse prescribers and other HCPs who are qualified to prescribe such as podiatrists, physios, paramedics etc.
Currently it is the prescriber who is responsible for assessing the patient and ultimately the treatment if it is done by a non-medical practitioner.
So, the question "who can perform Microsclerotherapy" is not a battle between doctors, nurses or aesthetic practitioners.
In my opinion, the controversy does not centre around who can inject but rather around “how can we ensure that people are appropriately selected, consented and treated in a safe environment with oversight by a healthcare professional.”
If you run your own aesthetic clinic, training your aesthetic practitioner how to inject leg spider veins under your supervision is a business-savvy way of leveraging your time.
As always, I am very interested to hear your views. Do you inject foam into leg spider veins? What do you think of compression afterwards?
If you are finding it difficult to grow a successful private medical or aesthetic practice, Veincare Academy may be able to help you.
Many thanks to the author of this blog Dr Haroun Gajraj who has over 30 years’ experience of treating people with varicose veins, thread veins and other vein complications such as phlebitis, varicose eczema and varicose ulcers.