Venaseal is the brand name for a form of ‘superglue’, chemically called cyanoacrylate, which is used in the treatment of vari cose veins.
cose veins.
It was originally formulated by a company called Sapheon, but they have now sold the Venaseal brand to a larger company called Medtronic. Venaseal is not the only ‘vein glue’ available on the market.
Venaseal bears a lot of similarities to the superglue you can buy in many shops to use in your own home. However, it has been specifically modified so that it can be used in medical practice. This is because it needs to be used within a vein and so does not set quite as rigidly as the commercial glue product. Therefore, when it has been used in a vein, you do not feel a rigid tube in your leg.Product Summary
Cyanoacrylate glue is a glue that is exceptionally good at gluing biological tissue together.
Anyone who has ever used superglue at home, and has accidentally glued their fingers together, knows quite how good it is gluing skin! (Do not try this at home!)
In the very early days of developing cyanoacrylate, experiments were done gluing different types of human tissue together including in liver surgery, and in closing skin incisions to avoid using stitches. However, because the market for selling glue products to use at home was bigger, most of the production went into producing superglue commercial sale, rather than in medical applications.
However, there have still been some uses for glue in medicine and biology which have been used for many years.
Venaseal was invented by Dr. Rob Rabe, an interventional radiologist in America. He used a similar glue to block off vessels that were bleeding, particularly in the case of brain aneurysms. He realised that if you could block off these high pressure vessels by injecting a glue down a very thin cannula, under x-ray control, then there was no reason you could not do this in bigger vessels such as varicose veins.
He then developed the cyanoacrylate polymer, which is a liquid/gel when injected into the vein and then hardens when in contact with fluid. He had to develop a compound of cyanoacrylate that was not rigid so that the treated vein did not feel like a "rod" in the leg whilst it was healing.
There have been a lot of research studies looking for any adverse effects of the cyanoacrylate glue in the body, but none have been found in humans. It appears to be very safe when used correctly by specialists who perform a lot of endovenous treatments, i.e. vascular surgeons who treat vein conditions.
As with all endovenous surgery for varicose veins nowadays, Venaseal is performed as a walk-in, walk-out, local anaesthetic procedure.
Having previously had your varicose veins diagnosed you would visit a specialist clinic for treatment to address the cause. Once changed out of your closes into surgical gowns, you will lie on the operating couch and the couch is tipped head up to fill the veins up in your legs. A vascular technologist marks where the main veins lie under the skin, using ultrasound, and then you stand up whilst the bulging veins on the surface are marked.
You will then lie back on the couch and your leg is cleaned with disinfectant fluid. Sterile operating sheets are placed around you and your leg. One local anaesthetic injection is then performed somewhere usually just above or below the knee. Under ultrasound guidance, a needle is passed into the vein. A wire is then passed up this needle, and the needle removed, leaving the wire in the correct position within the vein. Using this wire, a thin tube or catheter is passed up the vein, again under ultrasound control so the practitioner can see where it is going. It is placed just short of the top of the vein where it joins the deep vein.
The operating couch is then tipped head down to empty the vein of all blood. Pressure is applied to the top of the vein with the ultrasound tip. The surgeon injects a set amount of the Venaseal glue and pulls back the catheter. A period of time (usually three minutes) is then waited whilst the glue sets. This is important as this glues the vein shut.
The surgeon then injects a further set amount of glue, pulls the catheter back 3cm and waits another 30 seconds for the glue to start to set. This is continued for the whole length of vein that needs to be treated. Once the vein has been completely glued through the whole length, the catheter is removed and a little plaster is placed over the pinhole where the operation took place.
The use of Venaseal in an operation can be combined with other procedures, such as sclerotherapy, which may need to be done on other veins in the leg(s) during the same operating session, depending on the vascular problems that you have.
Your leg is usually placed in a support stocking and you will be asked to get up to walk about immediately (with assistance if required).
Venaseal glue should be used to close refluxing truncal veins such as the great saphenous vein, small saphenous vein and anterior accessory saphenous vein. Recent reports have also said it can be used for incompetent perforating veins using the TRLOP (TRansLuminal Occlusion of Perforators) technique.
It is not used for bulging (varicose) veins on the surface or for thread veins, although it might be used to treat the underlying veins which are causing such surface problems. It also might be used to cure the underlying veins causing venous eczema, swollen legs, brown staining around the ankles (haemosiderin) and leg ulcers.
It is important to note as with all endovenous (inside the vein) techniques such as endovenous laser ablation, radiofrequency ablation, TRLOP and MOCA (Mechanical Occlusion and Chemical Assistance), e.g. Clarivein, that all of these techniques treat the underlying refluxing veins (which are deeper inside the body) that cause things such as varicose veins, thread veins and skin damage that can be seen on the surface. They are not treatments for the varicose veins themselves, but they are essential to be used as part of the treatment for varicose veins and these other visible conditions.
Medical Device
As with all endovenous surgery including endovenous laser ablation, radiofrequency ablation, ultrasound guided foam sclerotherapy, TRLOP and MOCA, Venaseal should be used by teams of vein specialists as outlined in the National Institute of Health and Clinical Excellence (NICE) Guidelines CG168.
The consultant in charge of the team may be a vascular surgeon, general surgeon, interventional radiologist or occasionally a dermatologist but they will need to have a specialist understanding of endovenous surgery.
They should work as part of a team that include specialists that do the duplex ultrasound examinations to ensure correct diagnosis of the vein problem and safe and accurate placement of the catheter within the vein.
The NICE guidelines point out that this should always be performed as part of a team - although some doctors and clinics try to save money by having one doctor seeing the patient, doing their own scan and then doing the operation, this has been shown to reduce diagnostic accuracy and therefore is not recommended by the NICE guidelines.
Venaseal glue should not be used in surface veins where it might cause lumps that can be felt through the skin. It should also not be used in very large veins until research has been done to show that this is safe. It is probably less effective in veins that have had clot in them although once again, research is required to see if this is the case.
If this is performed properly by experienced endovenous surgeons working as part of a specialist team as recommended by NICE CG168, then a failure is very rare.
Research studies that have been done so far seem to indicate that the glue sticks the vein together in the first instance, but in the long term, the vein wall is permanently destroyed by what is called a "foreign body reaction". Once this has occurred, it is unlikely the vein will ever reopen in future.
Approximately one or two in every 10 people will suffer from "phlebitis" which is a painful red swelling running along the course of the treated vein. This occurs when there is a severe inflammatory action due to the vein being destroyed by the glue. It can also happen when veins that usually have blood flow into or out of the treated vein can become inflamed with phlebitis.
Sometimes, particularly with less experienced surgeons, or those without someone else doing the ultrasound scan whilst they are doing the procedure, the end of the catheter might not be precisely aligned and some of the glue might land into the deep vein. This looks like a very worrying consequence on the ultrasound, although it is probably not clinically relevant. There have not been any reports so far of this causing a clinical problem.
Although this is a very good system to reduce the number of injections needed to treat the underlying veins, if there are big bulging veins on the surface, they still need to be removed and so a lot of the advantage is lost. Venaseal has the biggest advantage in patients who do not like injections, but need to have underlying vein reflux treated when on the surface they have thread veins, small or very localised varicose veins, ankle swelling due to venous reflux but without visible varicose veins, venous eczema due to venous reflux but without visible varicose veins, or leg ulcers due to venous reflux but without visible varicose veins.
Venaseal is currently considerably more expensive than the more established endovenous laser ablation or radiofrequency ablation procedures.
When performed in the appropriate patients and correctly, the results should be the same with any of these three techniques. Therefore, in suitable patients, you will need to decide whether the extra cost of it is worth the reduction in the requirement to inject tumescent anaesthetic around the vein in multiple locations, which is needed in endovenous laser ablation and radiofrequency ablation procedures. Venaseal is less invasive in that respect.
Because of the cost, it is unlikely that private health insurance companies or the NHS are likely to fund a Venaseal procedure, although they may well do so in individual cases if a strong enough argument is made.
Expect to pay approximately £4,000 for treating one leg or £5,000 for treating both.
There has been a long-term study of which Professor Mark Whiteley was part of, looking at the efficacy of Venaseal in patients who had varicose veins due to great saphenous vein reflux, when the great saphenous vein was 10mm or less in diameter.
Several different vein centres around Europe were included and these patients have now been followed up for three years. The results have been excellent and have been reported in several meetings. In addition, a randomised controlled study published in 2015 (VeClose study) showed that in the short term, Venaseal glue and radiofrequency ablation success rates were almost identical. A further study called the WAVES study reported that success in treating the small saphenous vein or the anterior accessory saphenous vein was also excellent.
As such the Venaseal treatment for the treatment of great saphenous vein, small saphenous vein and anterior accessory saphenous vein appears to be equivalent in technical closure rates to endovenous laser ablation and radiofrequency ablation.
Photographs courtesy of The Whiteley Clinic and Venaseal™
(All before and after photographs are real patients, your results may differ).
Before and After Venaseal™ Treatment
Before and After Venaseal™ Treatment
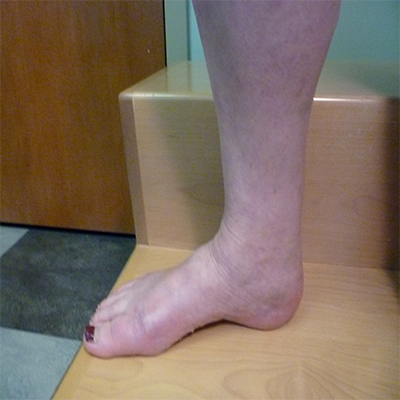
Before and After Venaseal™ Treatment
We would like to thank Vascular Surgeon Professor Mark Whiteley from The Whiteley Clinic for his expert medical help with this FAQ.