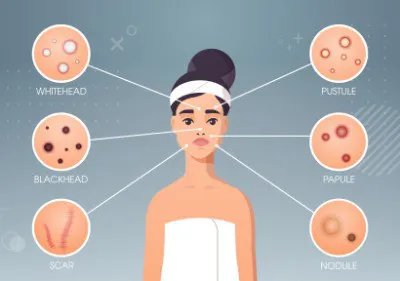
Acne is often discussed as if it were a single condition, yet in practice, it can present in several distinct ways. Some people experience mainly blackheads or small white bumps beneath the skin. Others develop red, inflamed spots or deeper lesions that take longer to settle. These differences are not random. They reflect changes taking place within the hair follicles, oil-producing glands, and surrounding skin.
Because acne can look different from one person to another, it is not always easy to recognise what type of acne is present or why certain treatments are recommended. Terms such as comedones, papules, pustules, nodules, or cysts may appear in medical advice, yet many people encounter these descriptions without a clear explanation of what they mean in practical terms.
Understanding the types of acne and their symptoms helps place these terms into context. It can also make it easier to recognise whether a breakout represents a mild form of acne, a more inflammatory pattern, or a condition that may resemble acne but develops for different reasons. This kind of knowledge supports more informed discussions with pharmacists, clinicians, or skincare professionals.
The first step in understanding acne is recognising why different lesion types develop and why dermatologists classify them in specific ways.
Our Preferred Partner - LDM® Triple
LDM® Triple is a non-invasive ultrasound-based treatment used in aesthetic and dermatology clinics to support skin health, tissue regulation, and the Treatment of Acne-Prone or inflamed skin. This guide is for anyone trying to understand what it is, how it works, and whether it may be relevant to their skin concern.
- What LDM® Triple is, and how it differs from standard cosmetic ultrasound
- Which skin concerns it is commonly used for, including Acne and early ageing-related concerns
- What to consider around suitability, comfort, risks, pricing and provider choice
Why Understanding Acne Types Matters
Understanding the types of acne can make a significant difference when deciding how to manage breakouts. Although many people refer to all spots as acne, dermatology recognises several different lesion types, each developing in slightly different ways within the skin.
Correctly identifying the type of acne helps guide treatment choices, whether that involves skincare adjustments, pharmacy treatments, or professional medical advice.
How Dermatologists Classify Acne
Dermatologists generally classify acne by lesion type and level of inflammation. This approach helps determine both the severity of the condition and the most appropriate treatment pathway.
In simple terms, acne is often divided into two broad categories:
-
Non-inflammatory acne, which includes blackheads and whiteheads
-
Inflammatory acne, which includes red, swollen spots such as papules and pustules
In more severe cases, acne can develop into deeper lesions, such as nodules or cysts, which sit beneath the skin's surface and may carry a higher risk of scarring.
These differences reflect what is happening inside the pore. Acne begins when excess oil (sebum), dead skin cells, and naturally occurring skin bacteria interact within the hair follicle. If the follicle becomes blocked but does not trigger inflammation, a blackhead or whitehead may form. When inflammation develops, the skin can produce red or pus-filled spots.
Healthcare professionals also consider:
-
Number of lesions present on the skin
-
Type of lesions, such as comedones, papules, or cysts
-
Location of acne, including the face, chest, or back
These factors help determine whether acne is mild, moderate, or severe, which in turn influences treatment recommendations.
Why Acne Types Can Affect Treatment Choices
Different acne types often respond to different treatment approaches.
For example:
-
Comedonal acne may respond well to topical skincare ingredients that reduce pore blockage.
-
Inflammatory acne may require treatments that reduce bacteria and inflammation.
-
Nodular or cystic acne sometimes needs prescription treatment or dermatology care to prevent scarring.
Clinical guidelines used in the UK also recommend reviewing acne treatment progress over a structured period, typically around 12 weeks, to determine whether the chosen approach is effective.
Understanding the type of acne present can therefore help set realistic expectations about how long treatment may take and whether professional advice may be useful.
Recognising the Variety of Acne Symptoms
Acne can appear in several forms, including:
-
Blackheads and whiteheads
-
Red inflamed bumps
-
Pus-filled spots
-
Deeper, painful lumps beneath the skin
These variations are normal and often occur together. A person may have more than one acne type at the same time.
Learning to recognise these differences can reduce confusion and make it easier to understand treatment advice offered by pharmacists, dermatologists, or aesthetic practitioners.
Although acne is extremely common, it is not a single uniform condition. Recognising the different types of acne lesions helps explain why breakouts vary from person to person and why treatment recommendations can differ.
Non-Inflammatory Acne: Blackheads And Whiteheads
Non-inflammatory acne is the mildest and most common type, and it usually appears as blackheads or whiteheads. These spots form when pores become blocked with oil and dead skin cells, but without significant inflammation or redness.
Although they may seem minor, these lesions often represent the earliest stage of acne and can sometimes develop into inflamed spots if the blockage inside the pore worsens.
Blackheads (Open Comedones)
Blackheads develop when a pore becomes blocked but remains open at the surface of the skin.
Key features include:
-
A small dark spot on the skin surface
-
Commonly found on the nose, chin, and forehead
-
Usually painless and not inflamed
The dark colour is often misunderstood. It is not caused by dirt, but by oil and dead skin cells inside the pore reacting with oxygen in the air.
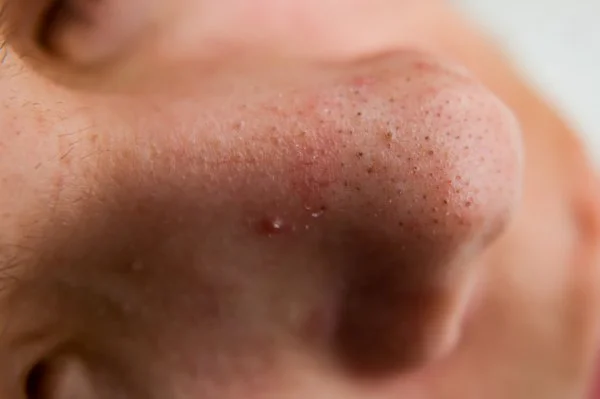
Blackheads are a form of acne known as open comedones.
Clinical considerations:
-
They often appear in areas with higher concentrations of oil-producing glands.
-
Over-cleansing or aggressive scrubbing may irritate the skin rather than improve blackheads.
-
Consistent skincare that supports normal pore turnover can help reduce recurrence.
Whiteheads (Closed Comedones)
Whiteheads occur when a pore becomes blocked but remains closed at the skin's surface.
Typical characteristics include:
-
Small white or flesh-coloured bumps
-
Smooth surface without redness
-
Often appearing on the forehead, cheeks, or jawline
These lesions are referred to as closed comedones.
They develop when:
-
Oil production increases
-
Dead skin cells accumulate inside the follicle
-
The pore opening remains sealed
Because the pore is closed, the trapped material stays beneath the skin surface, producing the characteristic white bump.
Clinical considerations:
-
Whiteheads may persist longer than blackheads because the pore remains sealed.
-
Picking or squeezing can irritate the follicle and increase the risk of inflammation.
-
Many topical acne treatments aim to reduce blocked pores and regulate skin cell turnover.
Why Non-Inflammatory Acne Can Progress
Blackheads and whiteheads may remain stable for long periods, but they can also develop into inflammatory acne.
This can occur when:
-
Bacteria within the follicle multiply
-
The blocked pore ruptures beneath the skin
-
The immune system triggers inflammation
When this happens, the skin may develop red bumps or pus-filled spots, which are considered inflammatory acne.
Blackheads and whiteheads are common signs of non-inflammatory acne, and they often represent the earliest stage of the condition. While they are usually mild, they can sometimes progress to inflamed lesions if the blockage within the pore worsens.
Inflammatory Acne: Red And Tender Spots
Inflammatory acne develops when a blocked pore triggers irritation and immune activity within the skin. At this stage, the follicle is not only clogged with oil and dead skin cells but also inflamed, leading to visible redness, swelling, and sometimes discomfort.
These lesions are more noticeable than blackheads or whiteheads and are often what people mean when they describe having "spots" or "breakouts".
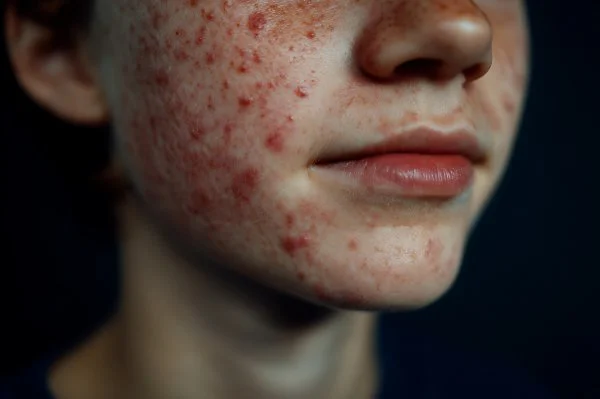
Papules
Papules are small red bumps that do not contain visible pus. They form when the wall of a blocked hair follicle becomes irritated and inflamed.
Typical features include:
-
Firm, red bumps on the skin
-
Tenderness when touched
-
No white or yellow centre
Papules occur when inflammation develops inside a blocked pore. The surrounding skin reacts as the immune system responds to the blockage and bacterial activity within the follicle.
Clinical considerations:
-
Papules often appear in clusters on the cheeks, forehead, or jawline.
-
They may last several days before resolving or progressing further.
-
Picking or squeezing can worsen inflammation and increase the risk of skin marks.
Pustules
Pustules are inflamed spots that contain visible pus at the centre of the lesion. They are commonly recognised as the classic "white spot".
Key characteristics include:
-
Red, swollen base
-
White or yellow centre containing pus
-
Often slightly raised above the skin surface
Although they resemble whiteheads, pustules differ because they involve inflammation and immune activity, not just a blocked pore.
Pus forms when immune cells gather within the follicle to respond to bacteria and irritation in the blocked pore.
Clinical considerations:
-
Pustules may resolve without scarring if left undisturbed.
-
Squeezing or picking can push inflammation deeper into the skin.
-
Repeated inflammation may increase the likelihood of post-inflammatory pigmentation or marks.
Why Inflammatory Acne Appears
Inflammatory acne often develops when a blocked follicle creates an environment where bacteria multiply. This process can trigger the skin’s immune response, leading to swelling and redness.
Common contributing factors include:
-
Increased oil production within the skin
-
Hormonal influences that stimulate sebaceous glands
-
Bacterial activity within blocked follicles
These processes explain why inflammatory acne may appear suddenly during hormonal fluctuations or periods of increased oil production.
Papules and pustules are the most common forms of inflammatory acne, and they develop when a blocked pore triggers inflammation in the surrounding skin. Although these lesions are usually temporary, repeated inflammation can increase the likelihood of marks or pigmentation changes.
Severe Acne Types: Nodules And Cysts
Some forms of acne develop deeper beneath the skin's surface, where inflammation affects larger areas of the follicle and surrounding tissue. These lesions are known as nodules and cysts, and they are generally considered the more severe types of acne.
Because the inflammation occurs deeper in the skin, these lesions tend to be larger, more painful, and slower to resolve. They may also carry a higher risk of scarring if left untreated.
Nodular Acne
Nodules are large, solid lumps that form beneath the skin’s surface. Unlike pustules, they do not contain visible pus.
Typical characteristics include:
-
Firm, painful lumps beneath the skin
-
Skin that appears red or swollen over the lesion
-
Spots that can remain for weeks rather than days
Nodules form when the wall of a blocked hair follicle ruptures deep within the skin. The resulting inflammation spreads into the surrounding tissue, producing a larger and more persistent lesion.
Clinical considerations:
-
Nodular acne often appears on the face, jawline, chest, or back.
-
Lesions may heal slowly and can leave marks or scars.
-
Over-the-counter treatments are often less effective because the inflammation occurs deeper within the skin.

Cystic Acne
Cystic acne represents one of the most severe forms of acne. These lesions develop when deep inflammation leads to the formation of large, pus-filled swellings beneath the skin.
Common features include:
-
Large, painful bumps beneath the skin surface
-
Soft or fluctuant swelling due to fluid and pus
-
Significant redness or tenderness in the surrounding area
Cystic acne often occurs in people with persistent or hormonally influenced acne, particularly along the lower face and jawline.
Clinical considerations:
-
Cysts can remain for extended periods and may recur in the same areas.
-
Because the inflammation occurs deep within the skin, there is an increased risk of permanent scarring or pigmentation changes.
-
Medical assessment may be helpful when these lesions recur frequently or fail to improve with standard acne treatments.
When Deeper Acne May Require Medical Advice
Deep nodules or cysts are often a sign that acne has progressed beyond the mild or moderate stage.
Professional assessment may be appropriate when:
-
Acne causes painful or persistent deep lesions
-
Spots repeatedly appear in the same areas
-
Early signs of scarring develop
-
Acne does not improve with standard topical treatments
Clinical guidance in the UK recommends reviewing treatment response over a structured period, often around 12 weeks, to assess whether a different treatment approach may be needed.
Nodules and cysts represent deeper forms of inflammatory acne. Because they occur beneath the skin's surface, they tend to be more persistent and carry a higher risk of scarring.
Hormonal Acne Patterns In Adults
Hormonal acne is a common pattern of breakouts that occurs when changes in hormone levels influence oil production in the skin. While acne is often associated with adolescence, many adults continue to experience breakouts well into their twenties, thirties, or beyond.
These patterns are particularly common in women and are often linked to natural hormonal fluctuations throughout the menstrual cycle.
Common Hormonal Acne Symptoms
Hormonal acne tends to appear in predictable areas of the face and may follow a recurring pattern.
Typical features include:
-
Breakouts concentrated along the jawline, chin, and lower cheeks
-
Spots that appear cyclically, often before menstruation
-
Deeper, tender lesions that can resemble nodules or cysts
-
Skin that feels oilier at certain points during the cycle
These patterns occur because hormones such as testosterone stimulate sebaceous glands, increasing the amount of oil produced in the skin. When excess oil combines with dead skin cells, it can block pores and trigger acne lesions.
Clinical considerations:
-
Hormonal acne may persist into adulthood even in people who did not experience severe acne as teenagers.
-
Breakouts may fluctuate with stress, sleep changes, or hormonal shifts.
-
Lesions are often deeper than typical teenage acne spots.
Hormonal Acne and Underlying Health Conditions
In some cases, hormonal acne may be linked to underlying medical conditions that affect hormone balance.
One example is polycystic ovary syndrome (PCOS), a condition that can influence hormone levels and increase oil production in the skin.
Signs that may suggest a hormonal component include:
-
Persistent acne concentrated along the lower face and jawline
-
Acne that continues into adulthood or begins after the teenage years
-
Breakouts that occur alongside irregular menstrual cycles or excess hair growth
When acne appears alongside these symptoms, healthcare professionals may consider a broader medical assessment.
Clinical guidance in the UK also recognises that certain medications, hormonal contraceptives, or hormonal changes during pregnancy may influence acne patterns.
Why Adult Acne Can Feel Different
Adult acne often behaves differently from teenage acne.
Common differences include:
-
Lesions may be deeper and more persistent
-
Breakouts may appear less frequently but last longer
-
Skin may also show signs of sensitivity or dryness from previous treatments
Understanding these patterns can help explain why treatment strategies for adult acne sometimes differ from those used during adolescence.
Hormonal acne is characterised by cyclical breakouts and deeper lesions, often concentrated along the lower part of the face. Recognising these patterns can help explain why acne sometimes persists into adulthood and why treatment approaches may vary.
Acne That Looks Similar But Is Not Acne
Not every spot or bump on the skin is acne. Several skin conditions can look similar to acne but develop for different reasons, so treatments for acne may not always be appropriate.
Understanding these differences can help prevent confusion and encourage people to seek appropriate advice if a skin concern does not behave like typical acne.
Rosacea
Rosacea is a long-term inflammatory skin condition that often affects the central areas of the face, particularly the cheeks, nose, forehead, and chin.
Common features include:
-
Persistent redness across the face
-
Visible small blood vessels
-
Red bumps that may resemble acne spots
One key difference is that rosacea does not produce blackheads or whiteheads, which are typical features of acne.
Clinical considerations:
-
Rosacea flare-ups can be triggered by heat, alcohol, spicy foods, or emotional stress.
-
Standard acne treatments may irritate rosacea-prone skin.
-
A healthcare professional can help distinguish between the two conditions during a skin examination.
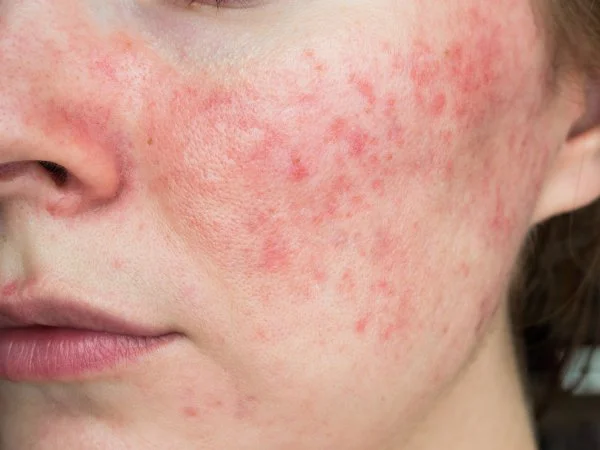
Folliculitis
Folliculitis occurs when hair follicles become irritated or infected, often due to bacteria, yeast, friction, or sweat.
It can appear similar to acne but tends to develop in areas where hair follicles are more easily irritated.
Typical characteristics include:
-
Small red or pus-filled bumps around hair follicles
-
Clusters of spots on the back, chest, shoulders, or buttocks
-
Skin that may feel itchy or tender
Clinical considerations:
-
Folliculitis can be triggered by tight clothing, shaving, or excessive sweating.
-
The condition may respond better to antimicrobial treatments rather than typical acne therapies.
Keratosis Pilaris
Keratosis pilaris is a common skin condition caused by keratin build-up inside hair follicles.
It is sometimes mistaken for acne, particularly when it appears on the arms or thighs.
Typical features include:
-
Small rough bumps that resemble goosebumps
-
Skin that feels dry or textured
-
Commonly affecting the upper arms, thighs, or buttocks
Clinical considerations:
-
Keratosis pilaris is not a form of acne.
-
The condition is usually harmless and often improves with moisturising and gentle exfoliation.
Why Accurate Identification Matters
Distinguishing between acne and other skin conditions is important because treatments are not interchangeable.
For example:
-
Acne treatments often target blocked pores and oil production.
-
Rosacea treatments focus on reducing inflammation and controlling triggers.
-
Folliculitis treatments may involve antimicrobial or antifungal approaches.
If a skin condition does not respond to typical acne treatments, a healthcare professional may consider alternative diagnoses.
Although acne is very common, several skin conditions can resemble it. Recognising the differences between acne, rosacea, folliculitis, and keratosis pilaris can help people understand their symptoms and seek appropriate care when needed.
How Acne Severity Is Assessed
When someone seeks acne advice, healthcare professionals usually assess the severity of the acne before recommending treatment. This assessment helps determine whether the condition is mild, moderate, or severe, and guides decisions about skincare, prescription treatments, or referral to a dermatologist.
Severity is not based on a single spot or breakout. Instead, clinicians consider the number and type of lesions and the areas of the body affected.
Mild Acne
Mild acne typically involves non-inflammatory lesions, with only a small number of inflamed spots.
Common features include:
-
Blackheads and whiteheads (comedones)
-
Occasional papules or pustules
-
Breakouts are usually limited to the face
Clinical considerations:
-
Mild acne often responds well to topical skincare treatments that help reduce blocked pores and oil production.
-
Over-the-counter ingredients such as benzoyl peroxide or azelaic acid are commonly used in early treatment approaches.
-
Consistent use of appropriate skincare is often more important than trying multiple treatments at once.
Moderate Acne
Moderate acne involves a greater number of inflammatory lesions and may affect more than one area of the body.
Typical signs include:
-
Frequent papules and pustules
-
Visible redness and inflammation
-
Breakouts affecting the face, chest, shoulders, or back
Clinical considerations:
-
Treatment may involve a combination of topical treatments and oral medication, depending on severity and response.
-
Healthcare professionals usually review treatment progress over a defined period to assess improvement.
Severe Acne
Severe acne includes deep inflammatory lesions, such as nodules or cysts, and often affects larger areas of the skin.
Key characteristics include:
-
Painful nodules or cysts beneath the skin
-
Widespread inflammatory acne
-
Increased risk of permanent scarring or pigmentation changes
Clinical considerations:
-
Severe acne often requires medical supervision and prescription treatment.
-
A dermatology referral may be considered if acne does not respond to initial treatment.
Clinical guidance used in the UK recommends reviewing treatment response after a structured treatment period, often around 12 weeks, to assess improvement and determine whether changes are needed.
Factors Clinicians Consider During Assessment
In addition to lesion type and severity, healthcare professionals may also consider:
-
Location of acne, such as the face, back, or chest
-
Duration of symptoms and whether acne is persistent or recurring
-
Signs of scarring or pigmentation changes
-
Whether acne is affecting psychological well-being or confidence
Acne can have a significant emotional impact on some people, which is also considered when deciding on appropriate treatment options.
Assessing acne severity helps healthcare professionals choose the most appropriate treatment approach and set realistic expectations for improvement. The type and number of lesions, as well as the areas affected, all play a role in determining whether acne is considered mild, moderate, or severe.
When Acne Symptoms Suggest Professional Advice May Help
Most people experience acne at some point, and many mild cases improve with appropriate skincare or pharmacy treatments. However, some acne symptoms may benefit from professional assessment, particularly when breakouts are persistent, painful, or affecting confidence.
Seeking advice does not necessarily mean a medical condition is severe. It simply allows a healthcare professional to evaluate the type of acne, its severity, and possible contributing factors before recommending treatment.
Persistent Acne That Does Not Improve
One common reason people seek professional advice is when acne does not improve despite consistent treatment.
Situations that may suggest further assessment include:
-
Acne lasting several months without improvement
-
Breakouts continue despite appropriate over-the-counter treatments
-
Spots returning quickly after treatment stops
Clinical guidance often recommends reviewing treatment progress after a structured period, typically around 12 weeks, as improvement may take time to become visible.
If acne does not improve during this period, healthcare professionals may recommend adjusting the treatment plan.
Painful or Deep Lesions
Professional advice may also be helpful when acne involves deep or painful lesions, such as nodules or cysts.
These types of breakouts:
-
It occurs deeper beneath the skin surface
-
May last longer than typical spots
-
Carry a higher risk of scarring
Early assessment can help reduce the likelihood of long-term skin changes.
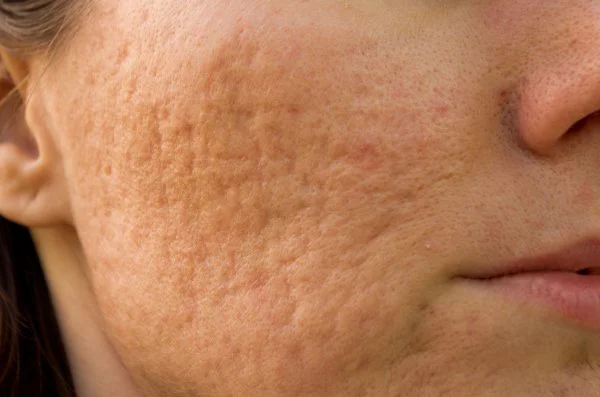
Signs of Scarring or Skin Changes
Another important reason to seek advice is when acne leaves visible marks on the skin.
These changes may include:
-
Indented or raised scars
-
Persistent red marks
-
Darker or lighter patches of pigmentation after spots heal
Repeated skin inflammation increases the risk of these changes developing, which is why early management can sometimes be helpful.
Acne That Affects Well-being
Although acne is a physical skin condition, it can also affect self-confidence and emotional well-being.
Some people experience:
-
Reduced confidence in social or professional settings
-
Increased concern about their appearance
-
Anxiety about long-term skin changes
Healthcare professionals recognise that the impact of acne can extend beyond the skin, and this may influence treatment recommendations.
What a Professional Assessment May Involve
A consultation for acne usually involves a visual skin examination rather than medical testing.
A healthcare professional may assess:
-
The type of acne lesions present
-
The distribution of breakouts across the face or body
-
Possible contributing factors such as hormones, skincare products, or medications
Based on this assessment, they may recommend:
-
Adjustments to skincare routines
-
Prescription medications
-
Dermatology referral in more persistent cases
Acne is extremely common, but persistent or deeper breakouts sometimes benefit from professional assessment. Early guidance can help identify the type of acne present and reduce the likelihood of longer-term skin changes.
Conclusion
Acne can appear in several different forms, from blackheads and whiteheads to deeper inflammatory lesions such as nodules or cysts. Recognising the types of acne and their symptoms helps explain why breakouts vary from person to person and why treatment recommendations may differ. Understanding whether acne is non-inflammatory, inflammatory, or linked to hormonal patterns can provide useful context when deciding how to manage the condition.
Another important point is that not every skin concern that resembles acne is actually acne. Conditions such as rosacea, folliculitis, or keratosis pilaris can look similar but may require different approaches. For this reason, identifying the pattern, location, and severity of breakouts is often the first step in choosing appropriate care.
If acne is persistent, painful, or causing lasting marks on the skin, it may be helpful to seek advice from a qualified healthcare professional who can assess the type and severity of the condition. For many people, taking time to understand how acne behaves and exploring reliable information sources is a sensible starting point before deciding on treatment.
Your Acne Questions
Real Questions from Real People — Answered
Straightforward answers to the questions people like you are asking right now about Acne.

Be the first to ask a Acne question.
Click here to ask your own question.
Find A Verified Clinic
Trusted Acne Experts, Local to You
Easily connect with qualified, verified professionals for safe, reliable treatment.


Akselberg Clinic
5 The Arcade , Hitchin, SG5 1EE
Welcome to Akselberg Aesthetics Our clinic is led by Dr Victoria Russell-Akselberg, an experienced practitioner in regenerative treatments with a background as an NHS surgeon.

Beauty Clinic Brazzini
185 Battersea High Street, Battersea Park, London, SW11 3JS
Beauty Clinic Brazzini is a boutique aesthetic clinic based in Battersea, London, specialising in advanced, non-surgical face and body treatments. Led by experienced practitioner Elisa Brazzini
To find a Acne clinic near you, please click here.