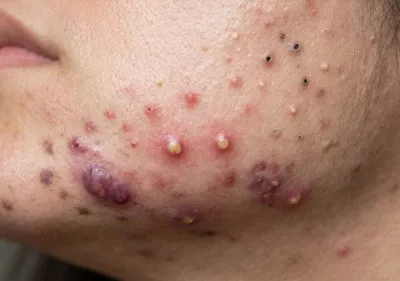
Acne is often discussed in simple terms, such as blocked pores or excess oil. In reality, it develops through a series of biological changes within the hair follicle. Oil production, skin cell turnover, bacterial activity and inflammation all play a role, and these processes can unfold gradually before a visible spot appears on the skin.
This complexity is one reason acne can feel difficult to interpret. Two people may experience similar breakouts but for different underlying reasons. Hormonal influences, skin type, genetics and environmental factors can all affect how acne develops and how severe it becomes. Because of this variation, treatment approaches often focus on addressing several stages of the process rather than one single cause.
Understanding how acne develops is helpful not only for recognising different types of breakouts but also for making sense of treatment recommendations. Many skincare products, medical treatments and professional procedures work by targeting specific stages in the acne cycle, such as reducing oil production, preventing blocked pores or calming inflammation.
To begin, it helps to understand the skin's basic structure and the small oil-producing glands where acne first develops.
Our Preferred Partner - LDM® Triple
LDM® Triple is a non-invasive ultrasound-based treatment used in aesthetic and dermatology clinics to support skin health, tissue regulation, and the Treatment of Acne-Prone or inflamed skin. This guide is for anyone trying to understand what it is, how it works, and whether it may be relevant to their skin concern.
- What LDM® Triple is, and how it differs from standard cosmetic ultrasound
- Which skin concerns it is commonly used for, including Acne and early ageing-related concerns
- What to consider around suitability, comfort, risks, pricing and provider choice
The Structure Of The Skin And Where Acne Begins
Acne develops beneath the surface of the skin, inside tiny structures called hair follicles. Understanding how these structures work helps explain why pores become blocked and why acne tends to appear in specific areas of the body.
Hair follicles and sebaceous glands: the starting point of acne
Each hair on the body grows from a hair follicle, a small tunnel-like structure within the skin. Attached to most follicles is a sebaceous gland, which produces an oily substance called sebum.
Sebum plays an important role in healthy skin:
-
It helps keep the skin soft and flexible.
-
It forms part of the skin's natural protective barrier.
-
It prevents excessive dryness by lubricating both skin and hair.
In people prone to acne, these glands can become more active and produce more sebum than the skin needs. The excess oil collects inside the follicle, creating conditions in which pores can become blocked.
Acne is most likely to develop in areas where sebaceous glands are more concentrated, including:
-
The face, particularly the forehead, cheeks and chin
-
The upper back
-
The chest and shoulders
These areas naturally produce more oil, which partly explains why breakouts tend to occur there.
Why does acne-prone skin produce more oil
Sebaceous glands respond strongly to hormones, particularly androgens such as testosterone. During hormonal changes, these glands can become more active and produce more sebum.
This helps explain why acne often develops during:
-
Puberty, when hormone levels increase
-
Menstrual cycles, when hormonal fluctuations occur
-
Pregnancy or hormonal changes in adulthood
In acne-prone skin, the glands may be especially sensitive to these hormones, even when hormone levels are within a normal range. This sensitivity leads to increased oil production and a higher likelihood of blocked pores.
Excess sebum then mixes with dead skin cells inside the follicle, forming the first stage of a blockage that can eventually develop into acne lesions such as blackheads, whiteheads, or inflamed spots.
The Four Biological Stages Of Acne Development
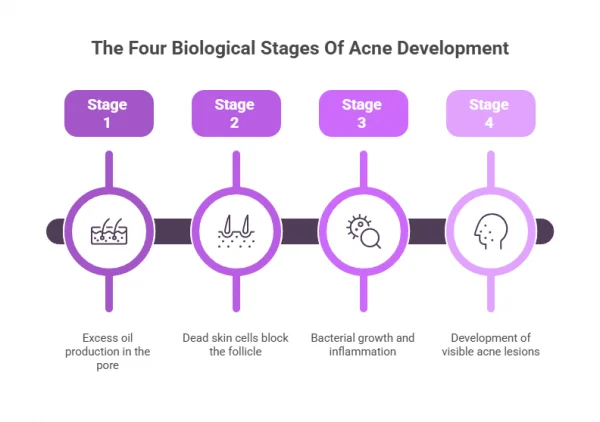 Acne does not appear suddenly on the skin. It develops through a series of biological changes inside the hair follicle, gradually progressing from excess oil production to visible spots on the skin.
Acne does not appear suddenly on the skin. It develops through a series of biological changes inside the hair follicle, gradually progressing from excess oil production to visible spots on the skin.
Understanding these stages can make treatment advice easier to interpret, as most acne treatments are designed to interrupt one or more of these steps in the process.
Stage 1: Excess oil production in the pore
The first stage of acne development begins when the sebaceous gland produces more sebum than the skin requires.
Several factors can contribute to this increase in oil production:
-
Hormonal changes, particularly during puberty
-
Hormonal fluctuations linked to menstrual cycles
-
Genetic predisposition to oilier skin
-
Increased sensitivity of sebaceous glands to normal hormone levels
As oil accumulates in the hair follicle, it creates an environment that makes the pore more vulnerable to blockage.
Excess sebum alone does not cause acne, but it is an important part of the process that enables the next stage.
Stage 2: Dead skin cells block the follicle
The skin naturally renews itself through a process called cell turnover. Dead skin cells are normally shed from the skin's surface without causing problems.
In acne-prone skin, this process can become disrupted. Instead of shedding cleanly, dead cells collect inside the follicle and mix with sebum.
This mixture gradually forms a plug inside the pore, which is known as a comedone.
Comedones may appear as:
-
Whiteheads, where the pore remains closed
-
Blackheads, where the pore is open and the material inside darkens when exposed to air
These early blockages are often the first visible signs of acne.
Stage 3: Bacterial growth and inflammation
The skin naturally contains bacteria, including Cutibacterium acnes. These bacteria usually live harmlessly on the skin.
However, when a follicle becomes blocked with oil and dead skin cells, the environment inside the pore changes. This trapped space allows bacteria to multiply more easily.
As bacteria increase, the body's immune system responds by triggering inflammation.
This inflammatory response leads to the development of:
-
Red bumps (papules)
-
Pus-filled spots (pustules)
-
Deeper inflamed lesions
Inflammation is what makes acne painful, swollen, or visibly irritated.
Stage 4: Development of visible acne lesions
As inflammation increases, the blocked follicle can expand or rupture beneath the skin. When this occurs, the contents of the follicle spread into the surrounding tissue, triggering a stronger inflammatory reaction.
At this stage, acne lesions may appear in several forms:
-
Papules: small red bumps
-
Pustules: spots containing visible pus
-
Nodules: larger, deeper inflamed lumps
-
Cysts: deeper lesions that can be painful and may increase the risk of scarring
The type of lesions that develop often reflects the severity of inflammation within the follicle.
More severe inflammatory acne can increase the risk of permanent scarring or changes in skin pigmentation, which is why early and appropriate treatment is often recommended.
Acne develops through a step-by-step biological process that begins inside the pore and gradually progresses to visible inflammation on the skin. Understanding these stages helps explain why treatments may take several weeks to show improvement.
Why Acne Severity Varies Between Individuals
Acne develops through similar biological processes in most people, yet its severity can vary widely. Some individuals experience occasional blocked pores, while others develop persistent or inflammatory acne that may require medical treatment.
Understanding the factors that influence acne severity can help explain why treatment plans differ between individuals.
Hormonal sensitivity and genetic predisposition
Hormones play an important role in regulating sebaceous gland activity. In some people, these glands are more sensitive to hormonal signals, leading to increased oil production and a higher likelihood of blocked pores.
Genetic factors can also influence how the skin behaves.
-
Acne often runs in families.
-
People whose parents experienced acne may be more likely to develop it themselves.
-
Genetic differences can affect oil production, pore structure, and inflammatory response.
Hormonal fluctuations are also a common reason why acne appears or worsens during certain life stages.
Examples include:
-
Puberty
-
Menstrual cycles
-
Pregnancy
-
Hormonal conditions such as polycystic ovary syndrome (PCOS)
These hormonal influences can increase sebum production and make acne more likely to develop or persist.
Skin type and pore characteristics
Differences in skin type can also affect the risk of acne.
People with naturally oilier skin tend to produce more sebum, increasing the risk of blocked pores. Larger or more active sebaceous glands can also contribute to congestion within the follicle.
However, acne is not limited to oily skin. Some individuals with combination or even relatively dry skin can still develop acne if other factors are present, such as:
-
Disrupted skin cell turnover
-
Hormonal influences
-
Pore blockage caused by skincare or cosmetic products
This is why acne treatment often focuses on regulating several skin processes rather than addressing oil production alone.
Lifestyle and environmental influences
External factors can also influence how acne behaves. These factors may not directly cause acne but can contribute to flare-ups or worsen existing breakouts.
Common examples include:
-
Stress, which can influence hormone levels
-
Certain skincare or cosmetic products that block pores
-
Friction or pressure on the skin, such as tight clothing or equipment
-
Heat and sweating, which can aggravate acne on the back and chest
-
Some medications, including steroid medicines or lithium
Lifestyle factors can vary significantly between individuals, which partly explains why acne patterns are different from person to person.
Acne severity is influenced by a combination of hormonal sensitivity, genetic predisposition, skin characteristics, and environmental factors. This variation is one reason why acne management often requires an individualised approach.
Why Acne Often Appears In Specific Areas Of The Body
Acne can develop anywhere hair follicles and sebaceous glands are present. However, it tends to appear more frequently in certain areas because these areas contain a higher concentration of oil-producing glands.
Understanding where acne commonly develops can help explain breakout patterns and guide appropriate treatment or skincare choices.
Facial acne and sebaceous gland density
The face contains one of the highest densities of sebaceous glands in the body. These glands produce sebum to protect and lubricate the skin, but increased oil production can make facial pores more likely to become blocked.
Breakouts commonly occur in areas such as:
-
The forehead, where oil production is often higher
-
The cheeks, where pores may become congested
-
The chin and jawline, which can be influenced by hormonal fluctuations
In adults, acne around the lower face and jawline is sometimes associated with hormonal patterns, particularly in women.
Facial acne may also be influenced by external factors, including:
-
Certain skincare or cosmetic products that block pores
-
Frequent touching of the face
-
Occlusion from face coverings or protective equipment
Choosing non-comedogenic skincare products and maintaining consistent cleansing habits can help reduce the risk of additional pore blockage.
Body acne on the back, chest and shoulders
Acne on the body, sometimes referred to as truncal acne, commonly affects the back, chest and shoulders. These areas also contain many sebaceous glands and can produce significant amounts of oil.
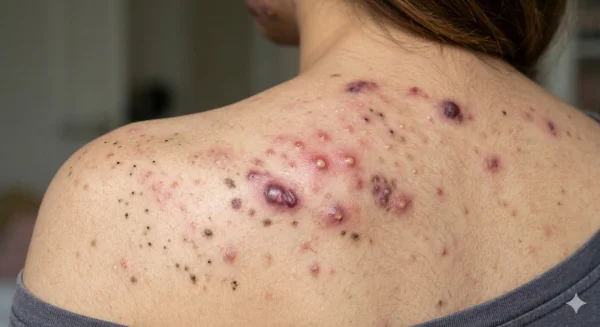
Several additional factors can contribute to acne in these areas:
-
Sweating, which can trap oil and dead skin cells on the skin
-
Friction from clothing or sports equipment
-
Tight or synthetic fabrics, which may increase heat and moisture
-
Difficulty applying topical treatments, particularly on the upper back
Because these areas are harder to reach, acne on the back and shoulders can sometimes persist longer without treatment.
It is also important to distinguish acne from other conditions that can appear similar, such as folliculitis, which involves inflammation of the hair follicles caused by infection or irritation.
Acne tends to develop in areas where sebaceous glands are most active and where oil, friction, or sweat can clog pores. Recognising these patterns can help guide appropriate skincare, lifestyle adjustments, or medical treatment when needed.
When Acne Becomes Inflammatory Or Severe
Acne can range from mild blocked pores to deeper, inflamed lesions that may affect the surrounding skin. Recognising when acne becomes more than occasional breakouts can help guide decisions about treatment and when to seek professional advice.
Signs that acne is progressing beyond mild breakouts
Mild acne typically involves blackheads and whiteheads, which are forms of blocked pores known as comedones. These lesions are usually small and may respond to consistent skincare or over-the-counter treatments.
Acne may be considered more advanced when inflammation becomes more prominent. Signs that acne is progressing can include:
-
Persistent red bumps (papules)
-
Pus-filled spots (pustules)
-
Larger, deeper lumps beneath the skin (nodules)
-
Clusters of inflamed spots that take longer to heal
Inflammatory acne can feel tender or painful and may appear suddenly when the blocked follicle triggers an immune response.
If breakouts become widespread, persist for several months, or begin to leave marks on the skin, a healthcare professional may recommend medical treatment.
Why deeper inflammation can increase the risk of scarring
Inflammation within the follicle can damage surrounding skin structures. When deeper lesions such as nodules or cysts develop, the inflammatory process may extend into the surrounding tissue.
This can increase the risk of:
-
Atrophic scars, which appear as small depressions in the skin
-
Raised scars, such as hypertrophic or keloid scars
-
Changes in skin pigmentation, particularly after the inflammation settles
Picking or squeezing spots can increase the likelihood of these complications, as it may push the contents of the follicle deeper into the surrounding skin.
Early treatment can help reduce the duration and intensity of inflammation, which is why persistent acne is often assessed by a healthcare professional. Acne is also recognised as a condition that can have psychological effects, including reduced confidence and anxiety, particularly when it is severe or long-lasting.
When acne becomes inflamed or persistent, the risk of longer-term skin changes such as scarring increases. Recognising these signs can help people seek appropriate treatment before complications develop.
How Understanding Acne Development Helps Guide Treatment Choices
Understanding how acne develops in the skin helps explain why different treatments are used and why a combination approach is often recommended. Most acne treatments target one or more stages of the acne process, such as excess oil production, blocked pores, bacterial activity, or inflammation.
This step-by-step approach is commonly used in dermatology and primary care, where treatments are usually reviewed after several weeks to assess improvement and tolerability.
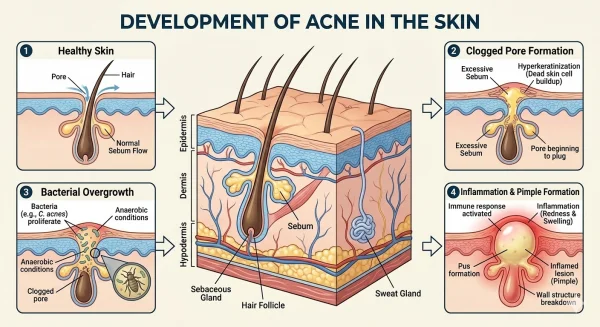
Treatments that target different stages of acne formation
Because acne progresses through several biological stages, treatment often focuses on interrupting those stages before inflammation worsens.
Common treatment approaches include:
Treatments that help prevent blocked pores
-
Topical retinoids such as adapalene or tretinoin
-
Products containing salicylic acid or azelaic acid
-
Skincare designed to support normal skin cell turnover
These treatments aim to reduce the build-up of dead skin cells within the follicle.
Treatments that reduce bacteria and inflammation
-
Benzoyl peroxide products
-
Topical antibiotic combinations prescribed by a healthcare professional
-
Oral antibiotics in certain cases
These approaches help reduce bacterial activity and calm inflammation within the follicle.
Treatments that address oil production and hormonal influence
-
Hormonal therapies in appropriate patients
-
Certain prescription medications that reduce sebaceous gland activity
In clinical practice, these treatments are often combined because targeting multiple stages of the acne process can improve outcomes.
Healthcare professionals usually review treatment progress after around 12 weeks, as visible improvement can take several weeks to develop.
Professional treatment options used in clinics
In addition to medical treatments and skincare, some individuals seek professional acne treatments from dermatology services or aesthetic clinics. These treatments are usually considered when acne is persistent or when additional support for the skin is required.
Examples may include:
-
Chemical peels, which help remove surface skin cells and support clearer pores
-
Light or laser-based treatments, sometimes used to reduce inflammation or bacteria
-
Ultrasound-based therapies such as LDM Triple, which are used in some clinics to support skin healing and inflammation control
-
Microneedling is occasionally used for acne scarring once active inflammation is controlled
These treatments are typically recommended following a consultation, where a practitioner can assess the type and severity of acne and determine whether professional procedures are appropriate.
Acne treatments work by targeting different parts of the acne development process. Understanding how acne forms can help make treatment plans clearer and explain why improvement may take time.
Conclusion
Understanding how acne develops in the skin can make the condition feel less confusing and easier to assess. Acne begins within the hair follicle, where excess oil, dead skin cells, bacteria and inflammation interact over time. This also explains why acne can look different from person to person, why some breakouts stay mild, and why others become more inflamed or harder to manage.
A few points are worth keeping in mind: acne is not simply a surface problem, severity is influenced by several factors rather than one single cause, and treatment usually works best when it targets the specific stage or pattern involved. That is also why improvement often takes time and why the right approach can vary between individuals.
If you are trying to better understand your own skin, it may help to read further in trusted UK clinical sources or speak with a qualified practitioner who can assess the type and severity of your acne in context. For many people, taking time to understand the process is a sensible first step in making informed decisions.
Your Acne Questions
Real Questions from Real People — Answered
Straightforward answers to the questions people like you are asking right now about Acne.

Be the first to ask a Acne question.
Click here to ask your own question.
Find A Verified Clinic
Trusted Acne Experts, Local to You
Easily connect with qualified, verified professionals for safe, reliable treatment.


Akselberg Clinic
5 The Arcade , Hitchin, SG5 1EE
Welcome to Akselberg Aesthetics Our clinic is led by Dr Victoria Russell-Akselberg, an experienced practitioner in regenerative treatments with a background as an NHS surgeon.

Beauty Clinic Brazzini
185 Battersea High Street, Battersea Park, London, SW11 3JS
Beauty Clinic Brazzini is a boutique aesthetic clinic based in Battersea, London, specialising in advanced, non-surgical face and body treatments. Led by experienced practitioner Elisa Brazzini
To find a Acne clinic near you, please click here.