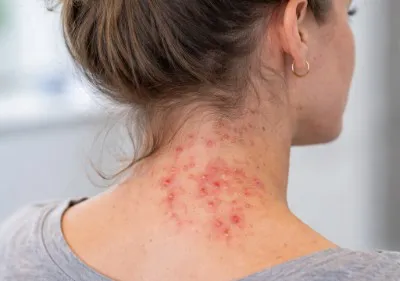
Neck acne can be easy to dismiss as a minor skin nuisance, but it often raises practical questions that are not always answered clearly. Some people are unsure whether they are dealing with acne at all, especially when spots appear alongside shaving irritation, ingrown hairs, redness, or sensitivity. Others want to understand why breakouts keep returning in the same area, particularly around the jawline, under the chin, or along the sides of the neck.
This matters because the neck sits between facial and body skin in both structure and exposure. It may be affected by hormones, sweat, friction, hair products, clothing, and skincare routines all at once. That can make the pattern less straightforward than acne on the forehead or cheeks. It also means that treatment is not always as simple as using a stronger product. In some cases, persistent neck acne may benefit from medical assessment, especially if it is painful, leaves marks, or does not respond to basic treatment.
This guide sets out the main causes of neck acne, how it differs from other skin conditions, and which treatment pathways are commonly used in the UK. It also explains what realistic treatment timelines look like, when clinic procedures may have a supporting role, and when it may be worth speaking to a GP, dermatologist, or qualified skin practitioner.
The first step is to understand what neck acne is and how it differs from occasional spots or other forms of skin irritation.
Our Preferred Partner - LDM® Triple
LDM® Triple is a non-invasive ultrasound-based treatment used in aesthetic and dermatology clinics to support skin health, tissue regulation, and the Treatment of Acne-Prone or inflamed skin. This guide is for anyone trying to understand what it is, how it works, and whether it may be relevant to their skin concern.
- What LDM® Triple is, and how it differs from standard cosmetic ultrasound
- Which skin concerns it is commonly used for, including Acne and early ageing-related concerns
- What to consider around suitability, comfort, risks, pricing and provider choice
Understanding Neck Acne
Neck acne refers to breakouts that develop on the skin below the jawline and around the sides or back of the neck. Although it may appear similar to facial acne, this area of skin is influenced by different factors, including friction, hormones, and irritation from clothing or grooming products.
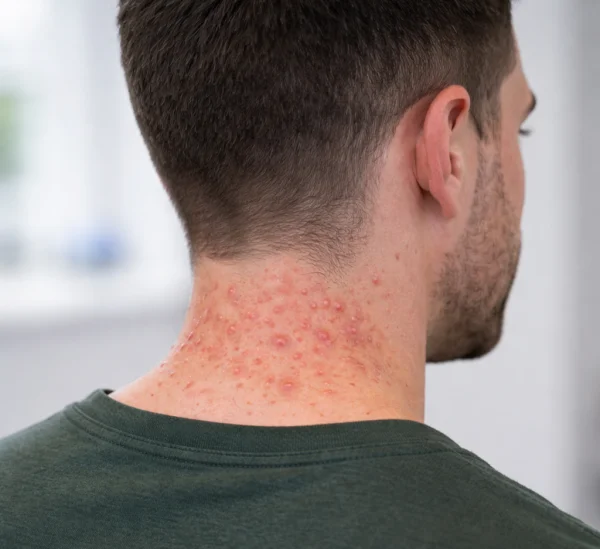
Understanding how neck acne develops can help explain why breakouts occur in this area and why they sometimes behave differently from facial spots.
What neck acne is and how it differs from occasional spots
Acne develops when tiny openings in the skin, known as hair follicles, become blocked with oil (sebum) and dead skin cells. Bacteria can then contribute to inflammation, which leads to the formation of visible spots.
Neck acne often includes a combination of:
-
Blackheads and whiteheads are caused by blocked pores
-
Red or inflamed spots known as papules or pustules
-
Deeper lumps under the skin, sometimes called nodules or cysts, in more severe cases
Occasional spots can appear anywhere on the skin and often resolve quickly. Persistent neck acne often involves recurrent breakouts in the same area, sometimes linked to hormonal changes or ongoing irritation.
Another difference is the structure of the skin in this region. The neck contains many hair follicles and sebaceous glands, but the skin barrier can be more easily irritated by shaving, clothing, or hair products. This combination can make breakouts more noticeable and sometimes slower to settle.
Common signs and symptoms of neck acne
Neck acne may appear in several ways depending on its severity and underlying triggers.
Common features include:
-
Clusters of small, inflamed spots, often along the jawline or sides of the neck
-
Tender or sore bumps that feel deeper than surface spots
-
Redness or irritation, particularly where clothing or collars rub against the skin
-
Post-inflammatory marks, which can appear as darker or red areas after a spot heals
In some cases, neck acne may also overlap with irritation caused by shaving or ingrown hairs. This can make it difficult to tell whether the underlying issue is acne, folliculitis, or simple skin irritation.
A healthcare professional can usually identify acne by examining the type of spots and where they appear on the body, including the face, chest, or back.
Neck acne is a common but often overlooked form of acne. Recognising how it forms and how it differs from occasional irritation or ingrown hairs is an important first step in choosing the most appropriate treatment approach.
Why Acne Often Appears On The Neck
Breakouts on the neck often develop for a combination of biological and environmental reasons. While the underlying acne process is similar to facial acne, the neck is exposed to additional triggers such as friction, shaving, and contact with hair or skincare products.
Understanding these factors can help explain why acne sometimes appears specifically along the jawline and neck rather than elsewhere on the face.

Hormonal influences on neck and jawline acne
Hormones play an important role in many cases of neck acne, particularly in adults.
During hormonal fluctuations, the sebaceous glands in the skin may produce more oil than usual. Excess oil can combine with dead skin cells and block hair follicles, creating the conditions for acne to develop.
Breakouts linked to hormones often appear along the:
-
Jawline
-
Lower cheeks
-
Neck and under the chin
This pattern is particularly common in adult women and may fluctuate with menstrual cycles or other hormonal changes.
In some cases, persistent acne around the jawline and neck may be associated with underlying hormonal conditions such as polycystic ovary syndrome (PCOS). When acne suddenly appears in adulthood alongside symptoms such as irregular periods or excessive hair growth, medical assessment may be recommended.
Friction, shaving and irritation triggers
The neck is an area where the skin frequently experiences mechanical irritation.
Common triggers include:
-
Clothing friction, such as tight collars, scarves, or sportswear
-
Shaving, which can irritate hair follicles or lead to ingrown hairs
-
Backpacks or straps rubbing against the sides of the neck
-
Sweat and heat, particularly during exercise or warmer weather
Repeated friction can disrupt the skin barrier and increase inflammation around hair follicles, which may contribute to acne-like breakouts.
This type of irritation is sometimes called "acne mechanica", where pressure or rubbing on the skin triggers or worsens existing acne.
Skincare and haircare products that may contribute
Products applied to the face, neck, or hair can occasionally clog pores.
Examples include:
-
Thick moisturisers or oils that sit heavily on the skin
-
Hair styling products transferring from hair onto the neck
-
Leave-in conditioners or hair serums contacting the skin
-
Certain cosmetic ingredients may block pores in acne-prone individuals
Many modern skincare products are designed to be non-comedogenic, meaning they are less likely to block pores. However, individuals with acne-prone skin may still react differently to particular formulations.
Reviewing products that regularly come into contact with the neck can sometimes help identify potential triggers.
A single factor rarely causes neck acne. Hormonal changes, skin irritation, and product build-up can all contribute to blocked follicles and inflammation in this area.
Neck Acne Vs Other Skin Conditions
Breakouts on the neck do not always mean acne. Several skin conditions can produce bumps, redness, or irritation in this area, and the treatment approach may differ depending on the underlying cause.
Recognising the differences between acne and other common conditions can help prevent unnecessary treatments and guide people towards appropriate care.
Folliculitis and razor bumps
Folliculitis is a condition in which hair follicles become inflamed, often due to bacterial infection, irritation, or ingrown hairs. It can appear very similar to acne, but it usually develops for different reasons.
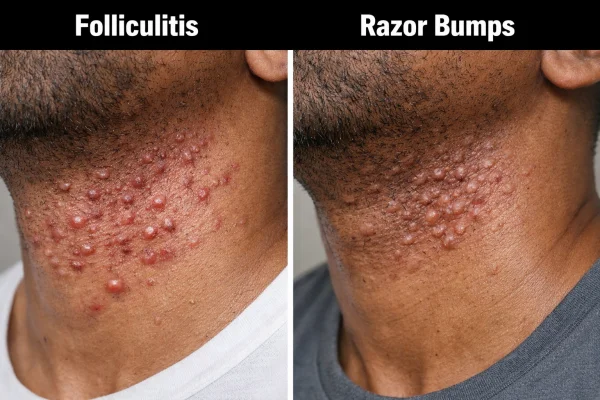
Common features of folliculitis include:
-
Small red or pus-filled bumps centred around hair follicles
-
Spots that may appear after shaving or friction
-
Clusters of bumps that can feel itchy or tender
Razor bumps, also known as pseudofolliculitis, occur when hairs grow back into the skin after shaving. This can trigger inflammation that resembles acne.
Key differences from acne may include:
-
Spots that appear directly after shaving
-
Bumps centred on individual hairs
-
More itching than deep inflammation
Because folliculitis and razor bumps have different causes, treatment may involve adjusting shaving techniques, reducing friction, or addressing bacterial infection rather than using typical acne medications.
Rosacea and other inflammatory conditions
Rosacea is another skin condition sometimes confused with acne. It most commonly affects the central areas of the face, but in some cases, redness or inflammation may extend towards the jawline or neck.
Typical rosacea features include:
-
Persistent redness or flushing
-
Visible small blood vessels
-
Sensitive or easily irritated skin
-
Fewer blackheads or whiteheads than in acne
Unlike acne, rosacea does not usually involve blocked pores. Treatment, therefore, focuses on reducing inflammation and managing triggers rather than targeting oil production or pore blockage.
Other inflammatory skin conditions, such as contact dermatitis, may also cause redness or bumps on the neck. These reactions are often linked to irritation from skincare products, fragrances, fabrics, or jewellery.
When a professional assessment may help
If breakouts on the neck do not respond to typical acne treatments, it may be helpful to seek professional advice.
A clinician can usually identify acne by examining the type of spots and where they appear on the body.
Medical assessment may be useful when:
-
Breakouts are painful or worsening
-
The diagnosis is unclear
-
Previous treatments have not improved symptoms
-
Skin irritation or redness is persistent
Accurate diagnosis helps ensure that treatment targets the underlying cause rather than the visible symptoms alone.
Several skin conditions can resemble acne on the neck. Understanding the differences between acne, folliculitis, and other inflammatory conditions can help guide appropriate treatment and avoid unnecessary irritation from unsuitable products.
Practical Steps That May Help Reduce Neck Breakouts
For many people, small adjustments to daily habits can help reduce irritation and support healthier skin. While these steps may not resolve persistent acne on their own, they can reduce common triggers that contribute to neck breakouts.
These practical measures are often recommended alongside medical or professional treatment where appropriate.
Gentle skincare routines for acne-prone skin
Consistent, non-irritating skincare can help support the skin barrier and reduce the likelihood of blocked pores.
Helpful approaches may include:
-
Cleansing the skin twice daily using a gentle, non-alkaline cleanser
-
Avoiding harsh scrubbing or abrasive exfoliants
-
Applying treatment products to the whole affected area rather than individual spots
Clinical guidance often recommends mild cleansing products and avoiding skincare formulations that block pores, particularly for people with acne-prone skin.
Products labelled non-comedogenic, or oil-free, are generally less likely to clog pores.

Clothing, exercise and hygiene considerations
The neck is exposed to friction, sweat, and pressure from clothing throughout the day. Reducing these factors may help limit irritation around hair follicles.
Practical steps include:
-
Wearing breathable fabrics, especially during exercise
-
Showering after physical activity to remove sweat and oil from the skin
-
Avoiding tight collars or scarves that rub against the neck for prolonged periods
-
Washing sportswear and gym clothing regularly
These measures help reduce the build-up of sweat and bacteria that may contribute to inflammation.
Avoiding picking and irritation
Although it can be tempting to squeeze or pick spots, this can worsen inflammation and increase the risk of long-term marks.
Skin picking may lead to:
-
Increased redness and swelling
-
Delayed healing
-
Post-inflammatory pigmentation
-
Potential scarring in more severe cases
Allowing spots to heal naturally while using appropriate treatments is generally the safest approach to protecting the skin.
Lifestyle adjustments and gentle skincare can help reduce some of the triggers that contribute to neck acne. However, persistent or inflamed breakouts may require targeted medical treatments to address the underlying causes.
Medical Treatments Used For Persistent Neck Acne
When neck acne continues despite basic skincare and lifestyle adjustments, medical treatment may be recommended. The choice of treatment usually depends on the severity of acne, the type of lesions present, and the individual's overall skin health.
In the UK, treatment often follows a stepwise approach. This typically begins with topical therapies and may progress to prescription medicines if acne does not improve.
Over-the-counter acne treatments
For mild neck acne, pharmacy treatments may be the first option.
Common active ingredients include:
-
Benzoyl peroxide, which helps reduce acne-causing bacteria and inflammation
-
Azelaic acid, which supports exfoliation and can help reduce redness
-
Niacinamide, which may help calm inflammation and support the skin barrier
These products are usually applied to the entire affected area rather than individual spots. This approach helps prevent new blockages from forming in nearby hair follicles.
It is important to recognise that acne treatments often take time to work. Improvement may take several weeks as the skin cycle gradually normalises.

Prescription treatments from a GP or dermatologist
When acne is more persistent or inflammatory, a GP or dermatologist may recommend prescription medication.
These may include:
-
Topical retinoids, which help prevent blocked pores
-
Combination topical treatments, such as retinoids with antibacterial agents
-
Oral antibiotics are used to reduce inflammation and bacterial activity
-
Hormonal treatments, sometimes considered for women with hormone-related acne
Treatment plans often combine topical and oral therapies. Clinical guidance typically recommends reviewing treatment after around twelve weeks to assess improvement and side effects.
Because antibiotics are involved in some treatment plans, healthcare professionals usually review their use carefully and limit long-term courses where possible.
When a dermatology referral may be considered
In some cases, referral to a dermatologist may be recommended.
This may happen when:
-
Acne is moderate to severe or causes scarring
-
Multiple treatments have not been effective
-
Acne has a significant psychological impact
-
More specialised treatments may be required
Dermatology-led care may include treatments such as isotretinoin or advanced therapies for severe acne.
Referral pathways can vary across NHS services and private dermatology clinics, but the aim is always to ensure that treatment is appropriate for the individual's skin and medical history.
Medical treatments for neck acne range from pharmacy products to prescription medicines. The most suitable option depends on the severity of acne, prior treatments, and individual skin characteristics.
Professional Clinic Treatments For Neck Acne
When neck acne persists despite skincare or medical treatment, some people explore professional procedures offered by dermatologists or aesthetic clinics. These treatments are usually used alongside a broader acne management plan rather than as a standalone solution.
A consultation with a qualified practitioner helps determine whether a procedure is suitable, particularly if acne is active or prone to scarring.
Chemical peels and resurfacing treatments
Chemical peels are commonly used in clinics to treat acne-prone skin.
These treatments typically involve applying a controlled exfoliating solution to the skin, which helps remove dead skin cells and clear blocked pores.
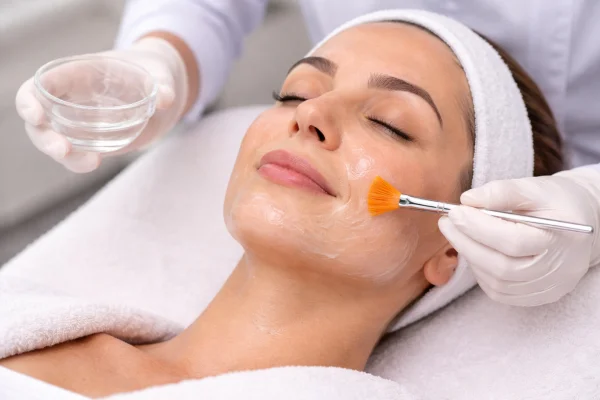
Potential clinical roles include:
-
Supporting exfoliation where pores are easily blocked
-
Helping reduce inflammation in mild to moderate acne
-
Improving the appearance of post-inflammatory marks left by previous breakouts
The strength and formulation of a peel are selected based on skin sensitivity and the severity of acne. Treatments are usually spaced several weeks apart to allow the skin to recover.
Light and energy-based treatments
Some clinics offer light-based or energy-based therapies designed to support acne management.
These treatments aim to:
-
Reduce the activity of acne-associated bacteria.
-
Calm inflammation within the skin
-
Support the skin's natural healing processes.
Light-based therapies may be considered when topical or oral treatments have provided only partial improvement and additional support is needed.
Suitability varies depending on skin type, acne severity, and whether active inflammation is present.
Ultrasound-based skin treatments such as LDM Triple
Low-frequency ultrasound treatments, such as LDM Triple, are sometimes used in aesthetic clinics as part of a broader acne management approach.
This technology uses alternating ultrasound frequencies that aim to support skin repair processes and reduce inflammation.
In clinical settings, practitioners may use ultrasound-based treatments to:
-
Support skin healing alongside other acne therapies.
-
Help calm inflamed skin.
-
Assist with recovery where the skin barrier has been disrupted
These treatments are generally considered supportive therapies rather than primary medical treatment for acne. A qualified practitioner can assess whether they are appropriate within an overall treatment plan.
Professional clinic treatments can complement medical therapies for neck acne by supporting skin renewal and reducing inflammation. Their role is typically supportive rather than curative, and they are most effective when used as part of a personalised treatment plan.
What To Expect From Acne Treatment
Treating neck acne usually requires a structured and consistent approach. While treatments can be effective, improvement often happens gradually rather than immediately.
Understanding how acne treatment typically progresses can help set realistic expectations and reduce frustration during the early stages.
Treatment timelines and realistic expectations
Most acne treatments work by gradually reducing blocked pores and inflammation within the skin.
Because the skin renews itself slowly, improvements usually appear over several weeks rather than days.
Typical timelines may include:
-
Early changes within 4 to 6 weeks, such as reduced inflammation or fewer new spots
-
Clearer improvement around 8 to 12 weeks as the treatment cycle continues
-
Longer-term management to prevent future breakouts
Clinical guidance often recommends reviewing acne treatments after approximately twelve weeks to assess effectiveness and adjust the plan if needed.
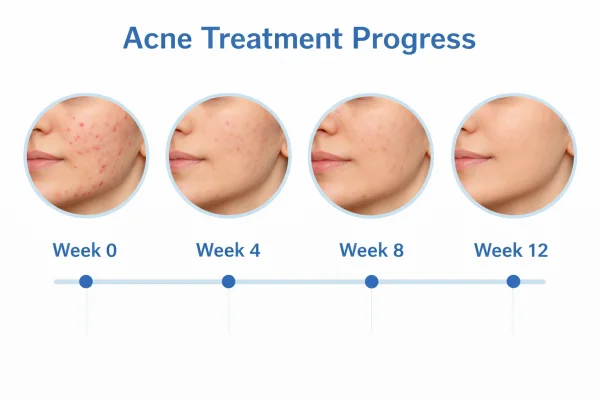
It is also common for certain treatments, particularly topical retinoids, to cause mild irritation or temporary worsening before improvement becomes visible.
Combining treatments for better outcomes
Many acne treatment plans involve combining different approaches rather than relying on a single product or procedure.
A comprehensive approach may include:
-
Topical treatments to reduce blocked pores and inflammation
-
Oral medication, where appropriate, to address deeper inflammatory acne
-
Skincare adjustments that support the skin barrier
-
Professional clinic treatments that complement medical therapy
Combining treatments allows practitioners to address several contributing factors simultaneously.
Preventing scarring and long-term marks
Early and consistent treatment can help reduce the risk of longer-term skin changes.
Preventive steps may include:
-
Treating acne early when breakouts become persistent
-
Avoiding squeezing or picking spots
-
Using sun protection to reduce the likelihood of pigmentation changes
-
Following treatment instructions consistently
Inflammatory acne can sometimes lead to changes in skin texture or pigmentation if left untreated. Addressing breakouts early helps reduce this risk.
Acne treatment is usually a gradual process that requires patience and consistency. With appropriate care, many people see steady improvement over time as inflammation settles and new breakouts become less frequent.
When To Seek Professional Advice
Occasional spots on the neck are common and often improve with basic skincare or pharmacy treatments. However, persistent or worsening neck acne may benefit from a professional assessment, particularly when the cause is unclear or previous treatments have been ineffective.
Seeking advice from a qualified healthcare professional can help confirm the diagnosis and identify a treatment approach suited to the individual’s skin and medical history.
Signs that acne may require medical assessment
Certain patterns of neck acne may indicate that medical guidance could be helpful.
Situations where professional advice may be appropriate include:
-
Breakouts that persist for several months despite using over-the-counter treatments
-
Painful, inflamed, or deeper spots, such as nodules or cysts
-
Acne that is leaving marks or scars on the skin
-
Sudden onset of acne in adulthood, particularly if other hormonal symptoms are present
-
Acne affecting confidence or well-being
A clinician can usually diagnose acne through a skin examination, identifying the types of spots present and where they appear on the body.
Early assessment can help prevent acne from progressing to more severe forms or causing long-term skin changes.
Preparing for a consultation with a clinician
A consultation for acne usually involves reviewing several factors that may contribute to breakouts.
A clinician may ask about:
-
Previous treatments, including pharmacy products or prescriptions
-
Current skincare and haircare routines
-
Lifestyle factors, such as exercise habits or clothing that may irritate the neck
-
Hormonal influences, including menstrual patterns in women
-
Medical history and current medications
This information helps build a clearer picture of the potential triggers for neck acne and supports a more personalised treatment plan.
In some cases, additional assessment may be recommended if hormonal conditions or other skin disorders are suspected.
Neck acne can often be managed with appropriate skincare and treatment, but persistent or severe breakouts may benefit from professional guidance. A clear diagnosis and tailored treatment plan can help reduce inflammation, prevent scarring, and support long-term skin health.
Your Acne Questions
Real Questions from Real People — Answered
Straightforward answers to the questions people like you are asking right now about Acne.

Be the first to ask a Acne question.
Click here to ask your own question.
Find A Verified Clinic
Trusted Acne Experts, Local to You
Easily connect with qualified, verified professionals for safe, reliable treatment.


Akselberg Clinic
5 The Arcade , Hitchin, SG5 1EE
Welcome to Akselberg Aesthetics Our clinic is led by Dr Victoria Russell-Akselberg, an experienced practitioner in regenerative treatments with a background as an NHS surgeon.

Beauty Clinic Brazzini
185 Battersea High Street, Battersea Park, London, SW11 3JS
Beauty Clinic Brazzini is a boutique aesthetic clinic based in Battersea, London, specialising in advanced, non-surgical face and body treatments. Led by experienced practitioner Elisa Brazzini
To find a Acne clinic near you, please click here.