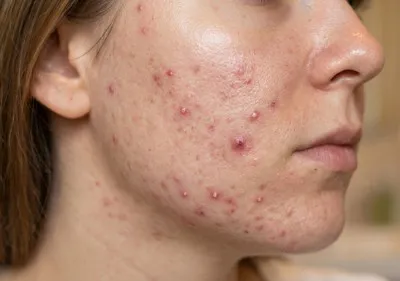
Acne is frequently discussed in everyday language as “spots” or “breakouts”, but medically it is a chronic inflammatory skin condition involving the hair follicles and oil-producing glands of the skin. Because it can present in several forms, from mild blackheads to deeper inflammatory lesions, people often find it difficult to determine what type of acne they are experiencing and whether treatment is needed.
Part of the confusion comes from the wide range of information available online. Advice about skincare routines, lifestyle changes, and professional treatments can sometimes overlap or conflict. At the same time, acne can affect people at different stages of life, including adolescence and adulthood, and may appear on areas of the body beyond the face. This variation means that what works for one person may not always be appropriate for another.
This guide explains the key processes behind acne, the different types of spots it can produce, where it commonly appears on the body, and why severity can vary between individuals. The aim is to provide a balanced overview that supports informed, low-pressure decision-making.
To begin, it helps to understand what acne actually is and why it is considered a medical skin condition rather than simply a collection of occasional spots.
Our Preferred Partner - LDM® Triple
LDM® Triple is a non-invasive ultrasound-based treatment used in aesthetic and dermatology clinics to support skin health, tissue regulation, and the Treatment of Acne-Prone or inflamed skin. This guide is for anyone trying to understand what it is, how it works, and whether it may be relevant to their skin concern.
- What LDM® Triple is, and how it differs from standard cosmetic ultrasound
- Which skin concerns it is commonly used for, including Acne and early ageing-related concerns
- What to consider around suitability, comfort, risks, pricing and provider choice
Understanding Acne: A Common But Often Misunderstood Skin Condition
Acne is one of the most common skin conditions worldwide, yet many people are unsure what it actually involves. In simple terms, acne develops when the skin’s hair follicles become blocked with oil and dead skin cells, leading to different types of spots.
The Medical Definition of Acne
Acne, often referred to as acne vulgaris, is a chronic inflammatory skin condition that affects the hair follicles and sebaceous glands.
Key characteristics include:
- Blocked pores are caused by a mixture of excess sebum (skin oil) and dead skin cells.
- The presence of different types of spots, such as blackheads, whiteheads, papules, pustules, nodules, or cysts.
- Inflammation is triggered by naturally occurring skin bacteria that multiply within blocked follicles.
- A tendency to affect areas with a higher density of oil-producing glands.
Acne most commonly appears on:
- The face, particularly the forehead, cheeks, chin and jawline
- The upper back and shoulders
- The chest
These areas contain more sebaceous glands, which explains why they are more prone to breakouts.
For many people, acne begins during puberty due to hormonal changes that increase oil production. However, it can also develop in adulthood and may persist for many years.
How Acne Differs from Occasional Spots
Most people experience the occasional spot, especially during hormonal changes or stress. Acne differs because it tends to be persistent and involves multiple lesion types across the skin.
Features that distinguish acne from isolated breakouts include:
- Recurring spots over weeks or months, rather than a single temporary blemish
- A mixture of different lesions, such as blackheads, inflamed spots, and deeper lumps
- Breakouts appearing across larger areas of skin rather than one isolated spot
- Potential for scarring or pigmentation changes if inflammation is significant
Understanding this distinction matters because occasional spots often respond to simple skincare adjustments, whereas acne may require structured treatment approaches that target oil production, blocked pores, and inflammation together.
Acne is not simply a matter of poor hygiene or isolated breakouts. It is a complex skin condition involving oil production, pore blockage, and inflammation. Understanding how acne forms is the first step towards recognising why treatments vary and why personalised care is often recommended.
How Acne Develops Inside The Skin
Understanding how acne develops in the skin can make the condition easier to manage and less confusing to treat. Acne does not begin on the surface of the skin; it develops deeper within the hair follicles, where oil production and skin cell turnover take place.
The Role of Sebaceous Glands and Oil Production
Sebaceous glands are small oil-producing glands connected to hair follicles. Their job is to produce sebum, an oily substance that helps keep the skin hydrated and protected.
In acne-prone skin:
- The sebaceous glands become overactive and produce more sebum than the skin needs.
- Excess oil begins to accumulate inside the follicle.
- Hormonal changes, particularly increases in androgen hormones during puberty, can stimulate this increased oil production.
- Some people naturally have sebaceous glands that are more sensitive to hormonal signals, which increases the likelihood of acne.
This excess oil creates an environment where acne can begin to develop.
How Blocked Pores Form
The next stage in the development of acne involves the lining of the hair follicle.
Normally:
- Dead skin cells shed from the follicle and rise to the surface of the skin.
In acne-prone skin:
- Dead skin cells accumulate and stick together inside the pore.
- These cells mix with excess sebum and form a plug within the follicle.
- If the pore remains closed, it forms a whitehead.
- If the pore opens at the surface, the oil and skin cells oxidise, forming a blackhead.
This early stage of acne is often referred to as comedonal acne.
The Role of Skin Bacteria and Inflammation
Human skin naturally contains bacteria that usually live harmlessly on the surface. One of these bacteria, Cutibacterium acnes, plays a role in the development of acne.
When a follicle becomes blocked:
- The trapped oil creates a low-oxygen environment where bacteria can multiply.
- The immune system reacts to this bacterial growth.
- This reaction triggers inflammation, causing redness, swelling, and tenderness.
As inflammation develops, the blocked follicle may become:
- A papule (a small red bump)
- A pustule (a pus-filled spot)
- In more severe cases, nodules or cysts, which form deeper within the skin.
This inflammatory process is what makes acne more visible, uncomfortable, and sometimes more difficult to treat.
Acne develops through a combination of excess oil production, blocked pores, bacterial growth, and inflammation within the skin. Because several processes are involved, effective treatment usually requires addressing more than one factor at the same time.
The Different Types Of Acne Spots
Acne does not appear as a single type of spot. Instead, it includes several lesion types, each reflecting what is happening within the skin and the extent of inflammation.
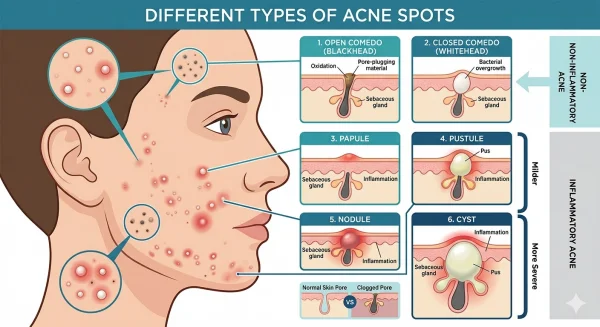
Recognising these differences helps explain why acne severity can vary and why treatment approaches may change depending on the type of spots involved.
Non-Inflammatory Acne: Blackheads and Whiteheads
These are often the earliest and mildest forms of acne. They occur when pores become blocked but have not yet developed significant inflammation.
Common features include:
- Blackheads (open comedones)
- The pore remains open at the skin surface.
- The dark colour is caused by oxidation of the material in the pore, not dirt.
- Most often appear on the nose, forehead, and chin.
- Whiteheads (closed comedones)
- The pore remains closed beneath the skin surface.
- A small white or flesh-coloured bump may be visible.
- These can develop into inflamed spots if the follicle becomes irritated.
Non-inflammatory acne, often called comedonal acne, is typically mild but can be persistent.
Inflammatory Acne: Papules and Pustules
When blocked follicles become inflamed, acne becomes more noticeable and sometimes tender.
These lesions include:
- Papules
- Small red or pink bumps on the skin.
- Caused by inflammation in the follicle.
- Usually firm to the touch and may feel slightly sore.
- Pustules
- Similar to papules but contain visible pus at the centre.
- Often described as the typical “white spot”.
- Caused by the body’s immune response to bacteria within the follicle.
Inflammatory acne can occur across the face, chest, shoulders, or back and may appear in clusters.
Severe Acne Lesions: Nodules and Cysts
In more severe cases, inflammation develops deeper within the skin.
These lesions include:
- Nodules
- Larger, solid lumps that develop deep within the skin.
- Often painful and slow to resolve.
- Can increase the risk of permanent scarring.
- Cysts
- Deep, inflamed lesions filled with fluid or pus.
- May resemble boils and can be tender.
- Typically require medical assessment and treatment.
Severe acne lesions are less common but usually require professional management, as they are more likely to cause long-term skin changes.
Acne includes a range of lesion types, from mild blocked pores to deeper inflammatory spots. Understanding these differences helps explain why acne severity varies and why treatment plans often need to be tailored to the individual.
Where Acne Commonly Appears On The Body
Acne most often develops in areas of the body where sebaceous glands are more active. These glands produce sebum, the natural oil that helps protect and lubricate the skin. When oil production is higher, the risk of blocked pores and inflammation increases.
As a result, acne tends to appear in predictable areas of the body, particularly those with a greater concentration of oil-producing glands.
Facial Acne
The face is the most common location for acne. This is largely due to the high number of sebaceous glands in facial skin.
Breakouts often appear in specific areas:
- Forehead - sometimes associated with excess oil production or hair products.
- Cheeks - may be influenced by skincare products, cosmetics, or friction from phones and hands.
- Chin and jawline - commonly linked with hormonal fluctuations.
- Nose and central face - an area where sebaceous glands are especially active.
Because facial skin is more visible and exposed to environmental factors, facial acne can also have a greater impact on confidence and daily routines.
Back Acne (Bacne)
The upper back is another area where acne frequently develops. This is sometimes referred to as bacne.
Contributing factors may include:
- A large number of sebaceous glands in the skin of the back.
- Sweat and friction, particularly during exercise.
- Tight or synthetic clothing that traps heat and moisture.
- Difficulty applying topical treatments evenly to the area.
Back acne can sometimes be more persistent because the skin in this area is thicker and harder to treat with topical products alone.
Chest Acne
Acne on the chest often appears in the upper chest area, where oil glands are also active.
Possible contributing factors include:
- Sweat and heat, particularly in warm environments or during physical activity.
- Friction from clothing or sportswear.
- Hormonal influences that increase oil production.
It is also important to recognise that some chest breakouts may be folliculitis, a different condition involving inflamed hair follicles, which can appear similar to acne.
Shoulder Acne
Shoulders are commonly affected alongside back acne.
Potential triggers include:
- Friction from clothing straps, bags, or sports equipment.
- Sweat accumulation during exercise.
- Oil transfer from hair products or conditioners.
Because the shoulders are exposed to both friction and oil, breakouts in this area can occur even when facial skin is relatively clear.
Neck Acne
The neck, particularly along the jawline and upper neck, can develop acne in some individuals.
Possible contributing factors include:
- Hormonal fluctuations affect the lower face and neck.
- Irritation from shaving or hair removal.
- Contact with hair products or styling products.
- Friction from collars, scarves, or protective clothing.
Neck acne may also overlap with other conditions, such as ingrown hairs or folliculitis, which sometimes require different treatment approaches.
Acne tends to appear in areas where oil glands are most active, including the face, back, chest, shoulders, and sometimes the neck. The location of breakouts can provide useful clues about potential triggers and may influence how treatment is approached.
Who Gets Acne And Why It Varies Between Individuals
Acne is often associated with teenage years, yet it can affect people at many stages of life. While hormonal changes play an important role, acne is usually influenced by a combination of genetic, hormonal, and environmental factors, which explains why experiences with acne vary so widely between individuals.
Teenage Acne and Hormonal Changes
For many people, acne first develops during puberty. This stage of life is characterised by significant hormonal changes that directly affect the skin.
Key factors include:
- Increased androgen hormones, which stimulate the sebaceous glands to produce more oil.
- Sebaceous glands that become more sensitive to hormonal signals during adolescence.
- A rise in sebum production makes pores more likely to become blocked.
- The combination of excess oil, dead skin cells, and bacteria leads to inflammatory spots.
Because these hormonal changes are part of normal development, acne during teenage years is extremely common.
Adult Acne and Hormonal Fluctuations
Acne can also appear or persist in adulthood. In recent years, dermatology services have reported an increase in the number of adults, particularly women, seeking treatment for acne.
Adult acne may be influenced by:
- Hormonal changes linked to the menstrual cycle, which can trigger breakouts in the days before a period.
- Hormonal conditions such as polycystic ovary syndrome (PCOS), which can increase androgen activity.
- Stress, which may influence hormonal balance and inflammatory responses in the skin.
- Lifestyle and environmental factors, including certain skincare products or occupational exposures.
Adult acne often appears along the lower face, jawline, and neck, although patterns can vary.
Genetic and Individual Skin Factors
Family history can also influence whether someone develops acne and how severe it becomes.
Important factors include:
- Genetic predisposition, meaning acne may run in families.
- Variations in sebaceous gland activity affect how much oil the skin produces.
- Differences in how quickly skin cells are shed inside the follicles.
- Individual immune responses to bacteria within blocked pores.
These differences help explain why some people develop only occasional breakouts, while others experience persistent acne that requires medical treatment.
Acne can affect teenagers and adults alike, and its development is rarely caused by a single factor. Hormones, genetics, and lifestyle influences all contribute to how acne appears and how long it lasts.
Why Acne Severity Can Vary
Not everyone experiences acne in the same way. Some people develop a few occasional spots, while others experience more persistent or inflammatory breakouts. Understanding how acne severity is classified helps explain why treatment approaches differ and when professional advice may be appropriate.
Mild, Moderate and Severe Acne
Healthcare professionals often describe acne using three broad severity categories. These categories are based on the type and number of spots present, as well as whether inflammation or scarring is developing.
- Mild acne
- Mostly blackheads and whiteheads.
- A small number of inflamed spots may be present.
- Often responds to topical treatments or pharmacy-based care.
- Moderate acne
- More widespread blackheads and whiteheads.
- A larger number of inflamed spots, such as papules and pustules.
- May require prescription treatments from a GP or dermatologist.
- Severe acne
- Numerous inflamed lesions, including nodules or cysts.
- Spots may be painful and develop deeper within the skin.
- Higher risk of scarring and pigmentation changes.
This type of classification helps clinicians decide which treatment options may be appropriate and whether referral to a dermatology specialist is needed.
Psychological and Lifestyle Impact
Acne is a physical skin condition, but it can also affect how people feel about their appearance and confidence.
Factors sometimes associated with acne severity include:
- The visibility of breakouts, particularly on the face.
- The presence of persistent inflammation or scarring.
- The length of time acne continues without improvement.
- The impact on self-esteem or daily activities.
For some individuals, these effects can be significant. Dermatology guidance recognises that the psychological impact of acne is an important factor in treatment decisions.
Acne severity can range from mild blocked pores to deeper inflammatory lesions. Recognising these differences helps explain why treatments vary and why early management can help reduce long-term skin changes.
Why Understanding Acne Matters Before Exploring Treatments
Before exploring acne treatments, it is helpful to understand what type of acne is present and how it develops in the skin. Acne is not a single condition with a single solution. It involves several biological processes, which means treatment often needs to address more than one factor simultaneously.
Taking time to understand the condition can help people make more informed decisions about skincare, medical treatment, and professional advice.
Why Acne Treatment Is Not One-Size-Fits-All
Acne treatments vary because acne can present in different forms and severity levels.
Factors that influence treatment decisions include:
- Type of acne lesions present, such as blackheads, inflamed spots, or deeper nodules.
- Severity of the condition, which may range from mild to severe.
- Location of acne on the body, for example, facial acne versus back or chest acne.
- Underlying triggers, including hormonal fluctuations, skincare products, or lifestyle factors.
Because of these variations, treatment approaches may involve different combinations of options.
These can include:
- Topical treatments, such as retinoids or benzoyl peroxide, target blocked pores and bacteria.
- Oral medications, including antibiotics or hormonal treatments prescribed by a GP or dermatologist.
- Professional skin treatments are sometimes used in clinics to support skin health and reduce inflammation. These may include procedures such as chemical peels, light-based treatments, or ultrasound-based therapies such as LDM Triple.
A personalised treatment approach helps address the underlying causes of acne rather than focusing only on visible spots.
Understanding how acne develops and how it varies between individuals helps explain why treatment plans are rarely identical. A careful assessment of skin type, acne severity, and potential triggers is usually the most reliable way to determine appropriate treatment options.
Your Acne Questions
Real Questions from Real People — Answered
Straightforward answers to the questions people like you are asking right now about Acne.

Be the first to ask a Acne question.
Click here to ask your own question.
Find A Verified Clinic
Trusted Acne Experts, Local to You
Easily connect with qualified, verified professionals for safe, reliable treatment.


Akselberg Clinic
5 The Arcade , Hitchin, SG5 1EE
Welcome to Akselberg Aesthetics Our clinic is led by Dr Victoria Russell-Akselberg, an experienced practitioner in regenerative treatments with a background as an NHS surgeon.

Beauty Clinic Brazzini
185 Battersea High Street, Battersea Park, London, SW11 3JS
Beauty Clinic Brazzini is a boutique aesthetic clinic based in Battersea, London, specialising in advanced, non-surgical face and body treatments. Led by experienced practitioner Elisa Brazzini
To find a Acne clinic near you, please click here.